What a day. What a day. I got up this morning and took Ashlynn to daycare. I got back home around 8 and my phone was ringing. It was MD Anderson asking if we could come earlier than 10:30. I had not yet packed our stuff because I figured I would have time to do it in the morning. I threw our stuff together (of course Ive already remembered several things I have forgotten) and we made it here by 10:00 and he was being wheeled back into surgery by 10:45.
Arriving for surgery
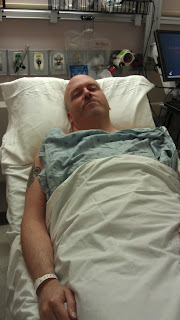
Very irritated because he has not eaten in 2 days and he is tired.....just ready to get started!!
Compression socks to prevent blood clots
Saints!!
Fixing to be wheeled away
Steve's brother, Stuart is in town from Mississippi. Stuart, me and my mom waited together for the surgeon to come give us the news. The surgeon came out about 2:45. He said, "why don't we go find a big room". I panicked for a quick second and then realized he probably can't sit and talk about Steve's surgery out in the open even if he wanted to. He must have sensed that that statement concerned us because he then turned around and said "he is fine". Anyhow, we got to the consultation room to speak with the surgeon, Dr. Lee. Dr. Lee said the surgery went well, but ended up being much more invasive than they originally planned for it to be. The tumor they removed (along with the adrenal gland) was the size of a softball. What made the surgery more invasive than originally planned was the fact that from the CAT scans there is no way to tell if the tumor is actually attached to other organs or touching other organs. Well, Steve had to go and do it BIG. His tumor was attached to his liver, kidney, AND the scariest of all the vena cava. So, since the tumor was attached basically everywhere, they had to take the surgery very slow. They slowly removed the tumor from the liver and kidney and then had to be extremely careful cutting the tumor from the vena cava. He had to have EIGHT blood transfusions during the surgery!! The surgeon said that most of the tumor appeared to be dead, but it will be sent off to the pathology for a full report. When we asked if they were able to remove it all in one piece or had to remove it in pieces, they said that they were able to remove it all in one piece but the tumor did rupture spilling "hopefully" dead tumor cells into the cavity. They were able to suction this up and "hopefully" this will not be a problem. He said with a tumor of this size there was basically no way to remove it without rupturing it or removing it in pieces. So, we will take what we can get. He did also say that he saw no evidence of melanoma (or any other type of cancer) anywhere else in the area he was in. So, that was great news!

Ever wonder what the different colored ribbons stand for?
Mom made me laugh. We were browsing the gift shop and she said she "would" buy me this card but I was with her, so I could just read it and take a picture :) Love you, Mommy!
We were originally told it would be 1-2 hours while Steve was in the recovery room and then we would be able to go back and see him. That 1-2 hours turned into about 4 hours. They could not get Steve's pain under control. The decision was made prior to surgery to administer pain meds and numb him through an epidural. Doing the epidural versus pain meds through an IV reduce side effects such as nausea and vomiting. When you have your belly sliced all up, the last thing you want to do is vomit! After FIVE attempts, they finally got the epidural working properly and Stuart and I were able to go back. (By this time, mom had to leave to pick up the kiddos).
Our first post-op look at Steve - no pain!!
Happy to have a pain med button!
A look at the incision
A close up of the incision
Steve and Stuart
Me and Steve <3
We visited with Steve and he was in good spirits. He was laughing, joking, showing us his incision, etc. Stuart left around 7-7:30 and shortly after that Steve started having pain. It went from a 4 to an 8 quickly. If the epidural was working properly, this should not be happening. I let the nurse know and she called anesthesia. Before anesthesia made it to the recovery room, Steve got transferred to an overnight recovery room that is basically more like an ICU room. By the time he got to the room, the pain had escalated from an 8 to a 10. Anesthesia finally got to the room and assessed the epidural. It was again leaking and not working properly, so he finally gave up on the epidural and is getting IV pain meds through a self administered pain pump. Unfortunately, he suffered at about a level 13 on the 1-10 pain scale for a good hour to hour and a half. He is still having some pain, but it is coming in waves and not quite as bad as it was. I am hoping he gets some rest tonight, but so far it doesn't look like it. Between alarms (his blood pressure keeps getting really low), nurses coming in, the pain, the narcotics, etc, he is just not able to get to sleep.













Dear sweet Jennifer. I had no idea you and your hubby were going through this! I will pray for a complete speedy recovery! I can't believe that incision! No wonder he is in so much pain! They need to keep it under control...no excuse for him to suffer. Love you! Nina Childress
ReplyDeleteThank you so much, Mrs. Childress. It has been a long hard road this last 6 months, but hopefully after this surgery and recovery our life we will get somewhat back to normal. Unfortunately, there is no cure for melanoma. So, even with this tumor removal Steve still has melanoma. Luckily it has not spread to many other areas and hopefully we can stay on top of those and get back to a normal life.
Deletepraying for you all!
ReplyDeleteThank you!!
DeleteYou're a great story teller, Jen. I'm relieved to hear the surgery was successful. Stay strong!!!
ReplyDeleteThanks, Jonathan :)
Delete